Microdiscectomy
Introduction
A lumbar microdiscectomy is an operation performed to decompress the nerve(s) in the lumbar spine by removing a disc prolapse via a small incision and minimal bone removal. In order for the operation to have the maximum chances of success there has to be good evidence of nerve compression in the lumbar spine (preferably with an MRI scan) with pain, weakness, or numbness in the leg or legs corresponding to the MRI findings
As described in the sciatica section, most patients with sciatica due to a disc prolapse will improve without surgery. This operation is usually performed if the sciatic pain has not responded to non-operative treatment such as physiotherapy, and the pain has persisted beyond 6-8 weeks. Other factors that may mean surgery is offered are if there is a profound weakness in the leg due to the disc prolapse, or in cases of very big disc prolapse

The image above an MRI scan of the lumbar spine, the red arrow indicates a disc prolapse on the left hand side ( scans are viewed as if you are looking from the feet up to the head). This type of disc prolapse is called a sequestered prolapse. This means that a fragment of the disc core has broken through the fibrous bag (annulus) containing it and has been squeezed out like toothpaste from a tube. The discs have a weak spot at the back and to the side, this also happens to be where the nerve root lies, and thus if the disc fragment is large enough the nerve root is compressed. Another type of disc prolapse is a diffuse prolapse, generally the annulus is intact in this type.
The Operation
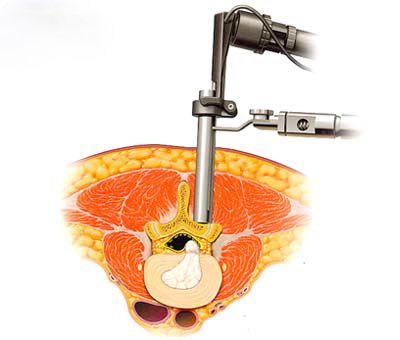
I have changed the way in which I operate on lumbar disc prolapse in recent years. Rather than cut the muscle from the bones to get to the spIne. I now split the muscles using a series of tubes to dilate a tract to the spine, or a similar retractor system, the operation is then performed via a tube or similar retractor, either using an endoscope or a microscope. This allows a very small skin incision to be used (16-18mm), and a more rapid recovery. Most patients operated on using this method go home the same day or stay one night in hospital.
The video below illustrates how the tubular system is used.
The conventional operation involves separating the muscle from the area to be explored, the muscle is preserved though, and only a minimal amount of dissection is performed. Overall if a minimally invasive approach is used, there does not seem to be a huge advantage of using the tubular retractors and thus I am flexible, and depending on the circumstances may use a more conventional retractor system.
Both approaches then result in the same procedure being performed on the disc and nerve root. Under the microscope (or endoscope), a window (fenestration) is made between the bone above and below by removing the yellow ligament (ligamentum flavum). Occasionally a small amount of bone needs to be removed if the space is narrow. The nerve root is then found, separated from the disc prolapse, and the disc prolapse removed. If the disc prolapse is a discrete fragment as in a sequestrated disc prolapse, then the fragment will be removed. The remainder of the disc will be explored for any other fragments that may prolapse, as much ‘normal’ disc is left behind to maintain the normal mechanics of the spine at this level. The aim of surgery is to remove the disc whilst retaining the normal structures that allow the stability and flexibility of the spine
Most patients are able to be admitted to hospital the morning of surgery having had nothing to eat or drink since midnight. The operation is performed under general anaesthesia with you lying on your front, an X-ray is performed at the beginning of the operation to localise the correct level in the spine.
The images below show the sequence of the operation. The first image is a normal lumbar vertebra / disc / nerve roots, the second shows a disc prolapse.


Below, a window (fenestration) is made in the ligament to access the disc prolapse


The video below illustrates the disc prolapse removal, again using the tubular system
As part of the operation I often perform a foraminotomy, this involves widening the canal where the painful trapped nerve leaves the spine, in addition to this I usually bathe the nerve root in a topical steroid at the end of the operation. The steroid seems to limit postoperative pain due to the nerve root swelling up as a reaction to being manipulated. At the end of the operation the wound is closed with dissolving stitches, the skin is closed with dissolving stiches and paper stiches, no drain is used.
Recovery From Surgery
Generally patients recover very quickly from this operation. Because the operation involves splitting rather than cutting only a very small area of muscle from the spine, back pain and stiffness after surgery is minimal and easily controlled with simple painkillers. We encourage patients to get up as soon as they are comfortable, usually with a few hours of surgery. This pain tends to be well controlled with painkilling medication such as ibuprofen, or a morphine-based medication. You will be encouraged to walk and use the bathroom with staff supervision as soon as possible, a physiotherapist will see you and supervise your mobilisation. Most patients are discharged home the same day or morning after surgery.
You can return to work when you fell comfortable, clearly this will depend upon how physically demanding your job is. In most cases 7-14 days off work is sufficient, if your job is physical then you may need up to 4-6 weeks off work. The DVLA state that you can drive when sufficiently recovered from surgery, in practical terms this means being able to look side to side and operate the car controls safely. Elderly patients may need additional support at home in the initial weeks after surgery. Thus, we would recommend getting additional family support if you are on your own at home, if this isn’t possible your GP may be able to organize some additional support for you
Results Of Surgery
The results of surgery are good with a 90+% rate of improving sciatica
The operation is not aimed at improving back pain, this is because the back pain usually originated from the degenerative changes in the spine and the changes due to wear and tear cannot be reversed with surgery. Some back pain due to muscle spasm may well improve however
The risks of surgery include, but are not limited to:
- The risks of a general anaesthetic ( this depends on your age and general health)
- Failure to improve your leg pain (less than 10% of cases)
- Leakage of spinal fluid from the spine (1%)
- Infection (1%)
- Damage to the nerve root or spinal nerves (very rare, in the order of 1 in 1000-2000), this can in theory result in weakness of
- the legs below the knees, and possibly incontinence
- Late instability of the spine (rare, more common in multiple level laminectomies, or previous surgery to the spine)